A third of all deaths in England and Wales are now linked to coronavirus, with fatalities occurring in people’s own homes more than tripling in one week.
The Office of National Statistics (ONS) said that of the deaths registered in the week ending April 10, 6,213 mentioned COVID-19, which is 33.6% of all deaths, compared with 3,475 in the previous week.
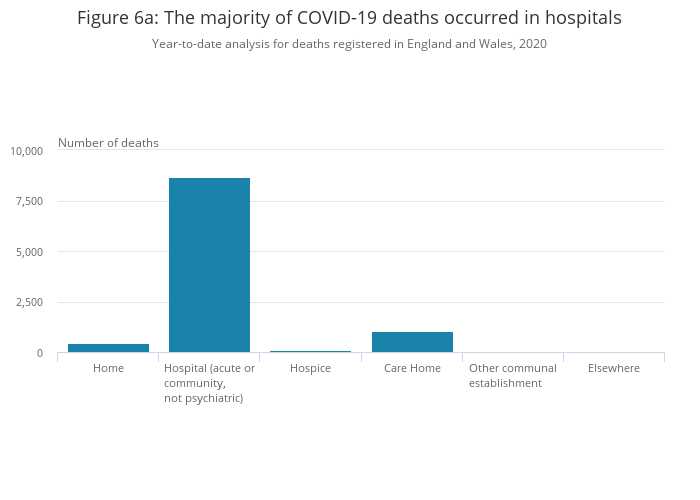
The figures show that the number of people confirmed to have died in their own homes from the virus rose to 466, up from 136 the previous week, while deaths in care homes increased fourfold to 1,043.
Publication of the figures comes amidst widespread criticism that the official figures are failing to reflect the true number of care home deaths, with Care England estimating they are closer to 7,500.
The CQC is working with the Office of National Statistics to explore how to provide a more detailed and timely picture of the impact of coronavirus on adult social care, using the data on deaths of people with suspected and confirmed COVID-19 that they collect from providers.
It said this will also give a regional view of which areas are being most impacted and may need additional support as a result. The data will be used to support weekly ONS reporting on deaths from April 28.
Ian Hudspeth, chairman of the Local Government Association’s Community Wellbeing Board said the “sad and shocking” figures highlight the “severe challenge” faced in care homes and other community settings.
“Council social care staff and care homes need urgent access to reliable and ongoing supplies of quality PPE, increased rapid and comprehensive testing and greater support with staffing and other equipment, on an equal footing with the NHS,” he added.
“Data on all deaths from COVID-19 needs to be published promptly and accurately, so we can have full confidence and transparency in these figures as part of our plan to defeat this deadly virus.
“We are also yet to see the peak of the stress on the social care system, due to the delay between hospital admissions and discharge, which will require the need to start thinking about shifting capacity across from hospitals and into the community to meet a surge in demand.”

